From intake to appointment: building trackable referral workflows

A referral is where intent meets reality. A clinician decides a patient needs specialty care, and suddenly the process depends on half a dozen systems, a handful of teams, and a “packet” of information that has to land perfectly for anything to move forward.
When that handoff works, patients get scheduled quickly, and providers stay aligned. When it doesn’t, care teams chase missing context, patients repeat themselves, scheduling slips, and the referral becomes a long thread of follow-ups.
This article lays out a practical model for building smarter referral workflows. We’ll define the referral lifecycle, map the failure modes, and share patterns that help teams ship improvements without taking on a full rebuild upfront.
What a referral is in healthtech terms
A referral is a structured handoff. One care team sends a patient to another provider, service, or facility for evaluation or treatment. In digital systems, a referral is best modeled as a workflow object that includes three layers:
- Clinical intent and expectations: why the referral is happening, what question needs answering, and what “success” looks like (consult only, co-management, or transfer of care).
- Patient readiness: clear explanation of the referral reason, what to expect next, and what the patient needs to do. This reduces drop-off and prevents the referral from turning into silent non-action.
- Operational and data flow: where the referral goes, what information must travel with it, and how status and outcomes return to the referrer.
Smarter referral workflows also treat packet requirements as a shared definition. Referrers and specialists align on what “good enough to act” means, so referrals arrive ready for triage and scheduling instead of triggering back-and-forth.
In practice, referrals behave like a lifecycle:
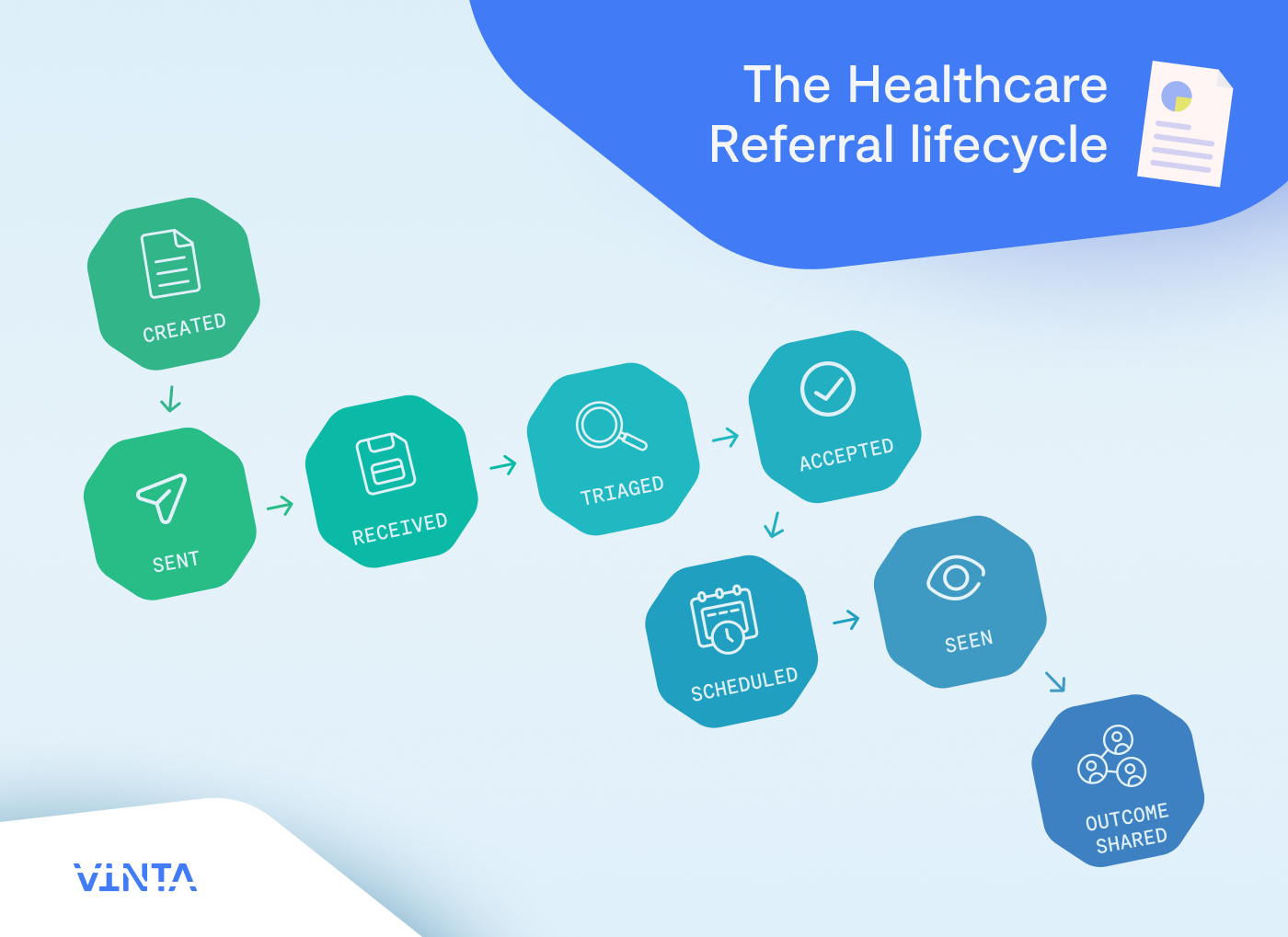
A workflow is closed-loop when the outcome, typically a consult note or structured result, reliably makes it back to the referrer and updates the original referral record.
When a system cannot represent and track that lifecycle, teams fall back to manual work. That is usually where the leaks begin.
Why referral workflows break
Referral friction is often blamed on “operations,” but most failures are predictable system behaviors.
1) Missing or inconsistent referral packets
The receiving team needs specific data to act. Referral notes may be there, but key context is missing. A lab result is in the EHR but not attached. Insurance info is captured but not mapped correctly. Staff fills gaps by calling offices, messaging patients, or asking for duplicate forms.
2) Status black holes
A referral is created and sent, and then it becomes unclear what happened. Care coordinators cannot see whether the referral was accepted, whether scheduling attempted outreach, or whether an appointment exists. Patients get contacted twice. Clinics assume the other side is handling it.
3) Identity matching and system boundaries
A patient exists in multiple systems with slightly different identifiers and demographics. The referral may be tied to one record while scheduling and billing use another. Attachments land in a document store that isn’t linked back cleanly. The end result is broader than “incomplete.” It can be inconsistent, duplicated, out of date, or attached to the wrong record entirely.
4) Payer requirements show up late
Eligibility checks, referral requirements, and prior authorizations are often triggered too late. If the intake data is wrong or if the ordering provider is not properly linked, payment gets delayed or denied.
5) Too many handoffs, too little ownership
Referrals touch clinical teams, call centers, schedulers, authorization staff, and specialist offices. If ownership isn’t explicit at each stage, work sits in limbo. The referral stops moving, patients wait without clear next steps, and teams spend time reopening the thread just to figure out who should act.
What “smarter” looks like
Smarter referral workflows share a few traits:
- They make the referral lifecycle visible to everyone who needs it
- They treat the referral as the source of truth for status, not a scattered set of tasks
- They enforce the minimum required data for triage and scheduling
- They trigger the right operational steps at the right time
- They log what happened so teams can debug failures and reduce repeat work
This is also where an integration-first approach earns its keep. Referrals tend to span EHR, scheduling, intake, document management, messaging, and billing. Rebuilding the full surface area takes longer and carries a higher rollout risk. Integrating what already exists, then replacing parts selectively, usually gets teams to measurable improvements faster.
Model the referral lifecycle as a first-class object
Start with a simple but explicit lifecycle model. It should include:
- Status: created, sent, received, triaged, accepted, scheduled, seen, outcome shared
- Events: actions that move the referral forward, such as documents received, patient contacted, appointment booked
- Ownership per state: care coordinator, scheduling team, authorization team, specialist office
- Required data per state: what must be present before scheduling can proceed
- Audit log: what changed, who changed it, when, and why
This does not require a new platform. It requires a consistent model that your systems agree on.
A practical rule: if a team has to ask “what is the status of this referral,” the system is missing a state or missing a signal.
Treat the referral packet like a product surface
When referrals break down, teams often discover two recurring drivers: the packet is not actionable when it arrives, and the handoffs are not well-instrumented. Improving packet quality tends to reduce downstream churn quickly.
Define a minimal referral packet per specialty and use case. Keep it small enough to be realistic and strict enough to reduce back-and-forth.
Examples of common requirements:
- Demographics and contact details
- Insurance subscriber info and coverage snapshot
- Referring provider NPI and contact
- Clinical reason for referral and urgency
- Referral intent/type: consultation-only (advice), co-management, or transfer of care, plus the specific question to answer.
- Recent notes that justify the referral
- Supporting labs, imaging, and medications
- Any prior authorization or referral ID if required (if applicable): whether the plan requires a referral or prior auth, and what is known so far. When an auth ID exists, capture it. When it can’t exist yet, capture what the specialist needs to initiate it after triage or the first evaluation.
Then implement two guardrails:
- Validation at creation: do not let incomplete referrals enter the system.
- Missing-data workflows: if something is missing, trigger the right task immediately.
This is where many teams use intake tooling effectively. You can keep vendor-hosted intake pages to collect structured information, then wire it into the referral lifecycle.
Connect intake and orchestration without rebuilding patient-facing UI
A common, pragmatic pattern is:
- Use Digital Intake hosted pages for patient-facing forms and document collection
- Use a workflow engine like Awell to orchestrate referral-related tasks and follow-ups
- Keep your referral lifecycle as the trackable object that ties everything together
Hosted pages help you move quickly on the patient-facing steps. Your team avoids building forms, signature flows, and edge-case validation in the first iteration. Meanwhile, orchestration ensures staff tasks happen consistently, and the referral status stays current.
This approach works best when you define:
- Which system is the source of truth for each piece of data
- How updates are propagated back to the referral lifecycle
- What happens when events fail or arrive out of order
Make the workflow measurable from day one
If you can measure it, you can improve it. Referral workflows benefit from a few practical metrics:
- Time from referral created to appointment scheduled
- Percentage of referrals that reach closed-loop completion
- Leakage rate (referrals created but never scheduled or never completed)
- Manual touches per referral (calls, messages, record requests)
- Percentage of referrals missing required documents at creation
- Patient drop-off rate during handoff steps
These metrics give product teams and operations leaders a shared language. They also help you justify future integration work.
Where reimbursement risk shows up
Referral workflows often sit close to revenue integrity. Breaks in data flow can cause:
- Delayed or failed eligibility verification
- Missing referral documentation required by the plan
- Prior authorization steps triggered too late
- Mismatched provider identifiers or patient identifiers
- Missing clinical documentation for medical necessity
You do not need to solve every payer edge case in v1. You do need to identify which referral types are most sensitive and build guardrails around those data fields and workflow steps.
If reimbursement is a major concern for a specific specialty, build a “payer readiness” checklist into the workflow so staff see what is still missing before scheduling proceeds.
A phased roadmap that works in real orgs
Most teams try to fix referrals by replacing everything at once. The better path is phased.
Phase 1: Quick wins
- Define the referral lifecycle states and the minimum referral packet
- Add validation rules at referral creation
- Create a basic status view for teams
- Standardize intake for the highest-volume referral type
- Keep hosted intake pages if needed for speed
Phase 2: Integration-first
- Wire bidirectional updates between your referral system and the EHR
- Automate document requests and attachment linking
- Trigger triage, outreach, and authorization tasks reliably
- Reduce duplicate entry across scheduling and intake
Phase 3: Closed-loop maturity
- Implement reliable feedback to referring providers
- Improve patient transparency with clear next-step messaging
- Add analytics for bottlenecks by specialty, clinic, or payer
- Harden identity matching and auditability
This roadmap gives leaders a safe way to fund progress and reduce risk. It also gives product teams a sequence that keeps delivery momentum.
A checklist for product teams
If you are building or modernizing referrals, these questions usually surface the real gaps:
- Can every team see the current referral state and the next owner?
- Do we enforce a minimum referral packet before handoff?
- Are eligibility, referral requirements, and auth steps triggered early enough?
- Do we have a clear source of truth for referral status?
- Can we trace why a referral got stuck, with an audit log?
- Are patient-facing steps fast to ship and maintain?
- Are we measuring time-to-schedule, leakage, and manual touches?
- Are we aligning our packet and referral intent fields with common referral templates and guidance (for example, CMS and AAFP-style referral templates), so referrers and specialists share expectations?
If the answer is unclear on more than a couple of these, the workflow is already costing you more than it should.
How we can help teams improve referrals
If you’re building or modernizing referral workflows, we’re a solid partner to help you get it right in specialty care operations. That often means integrating intake tools and workflow orchestration, establishing a clear referral lifecycle model, and shipping improvements in phases so teams see impact early.
If your referral workflow is slowing down specialty access or creating operational drag, we can help you map the lifecycle, define the data model, and build a plan that improves reliability without stalling delivery.

.webp)










%201.webp)
